The Pulse on Perfusion: Simulation, Animal Testing, and the Future of Training

As 2026 continues to bring rapid advances in technology, this month’s Pulse on Perfusion turns to a question many in the field are actively grappling with: how far can simulation go, and where do animal models still play a role? At Perfusion.com, this poll explores the intersection of ethics, education, and clinical readiness – areas where decisions are rarely simple and often deeply personal. With many perfusionists having trained on animal models themselves, the responses reflect not just opinions but lived experience. What emerges is a thoughtful and at times divided conversation about what the future of perfusion training should look like.
Poll Results at a Glance
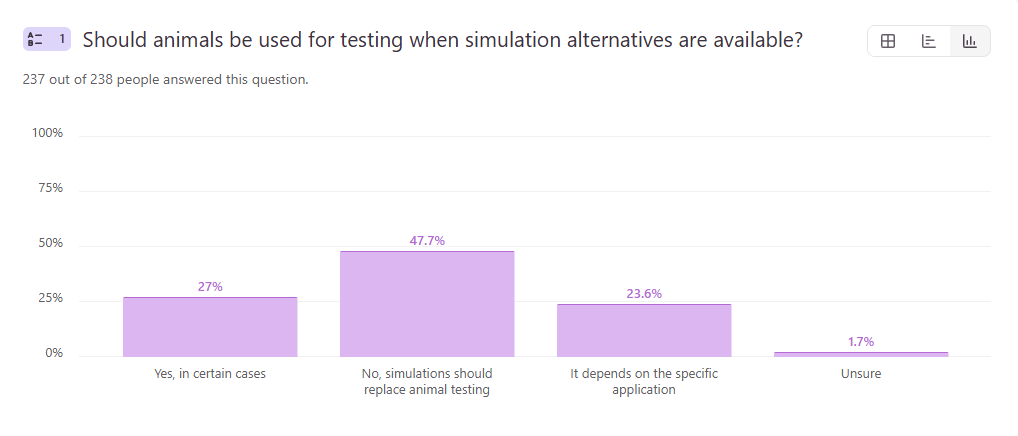
Question 1: Should animals be used for testing when simulation alternatives are available?
- No, simulations should replace animal testing – 47.7%
- Yes, in certain cases – 27.2%
- It depends on the specific application – 23.4%
- Unsure – 1.7%
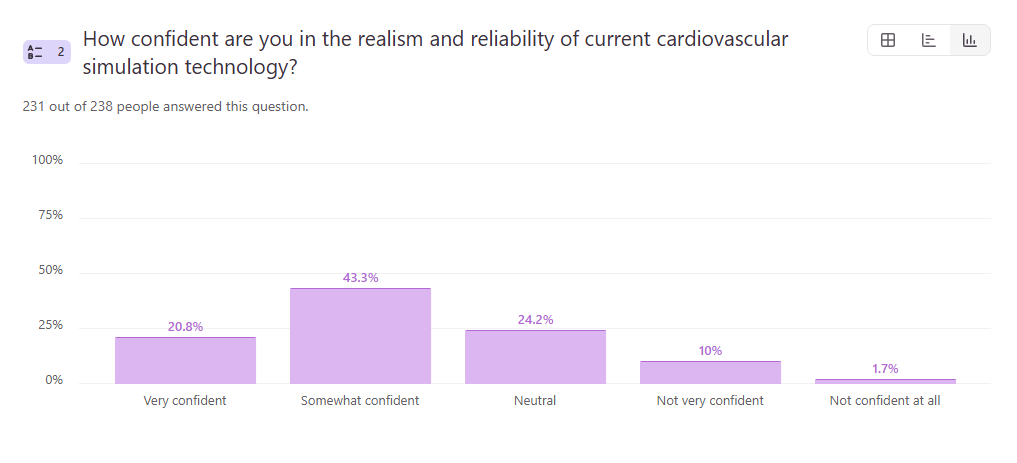
Question 2: How confident are you in the realism and reliability of current cardiovascular simulation technology?
- Somewhat confident – 43.2%
- Neutral – 24.5%
- Very confident – 20.5%
- Not very confident – 10%
- Not confident at all – 1.8%
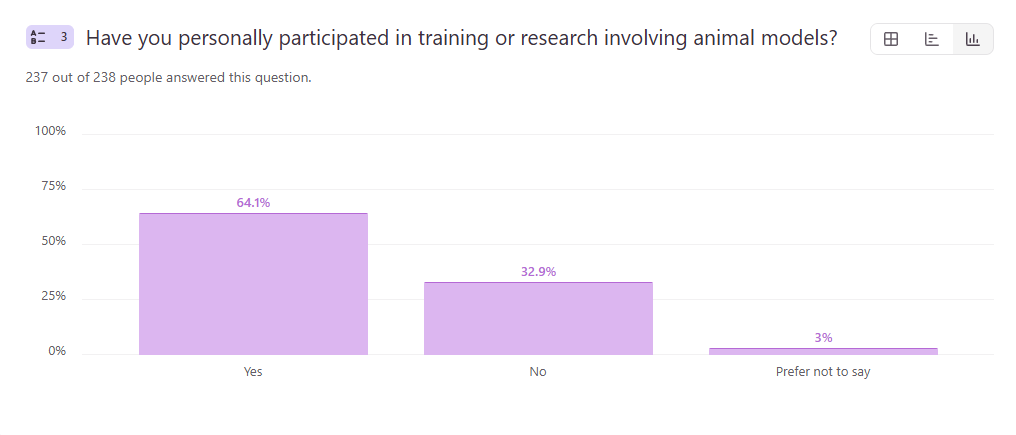
Question 3: Have you personally participated in training or research involving animal models?
- Yes – 63.8%
- No – 33.2%
- Prefer not to say – 3%
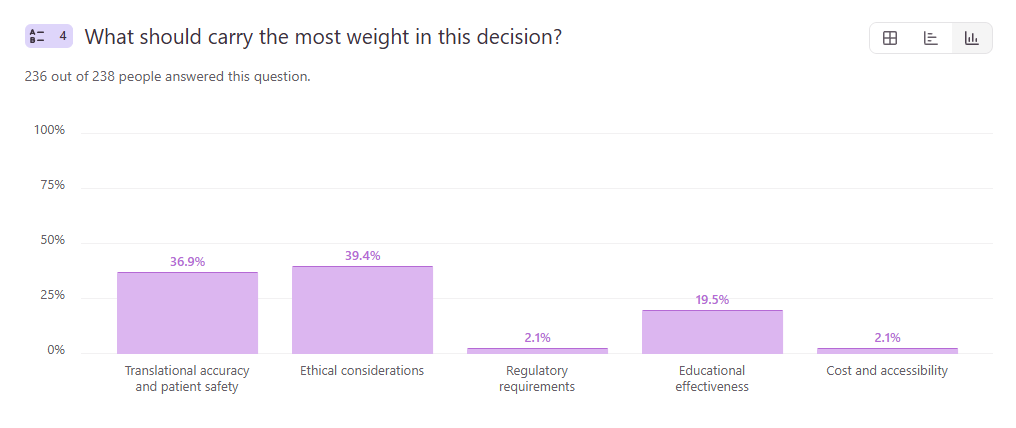
Question 4: What should carry the most weight in this decision?
- Ethical considerations – 39.7%
- Translational accuracy and patient safety – 36.8%
- Educational effectiveness – 19.2%
- Regulatory requirements – 2.1%
- Cost and accessibility – 2.1%
The respondent base skews toward experienced professionals, many of whom have direct exposure to animal-based training. This adds important context to how simulation is evaluated, not just as a concept, but as a comparison point against real-world experience.
Responses by Job Title
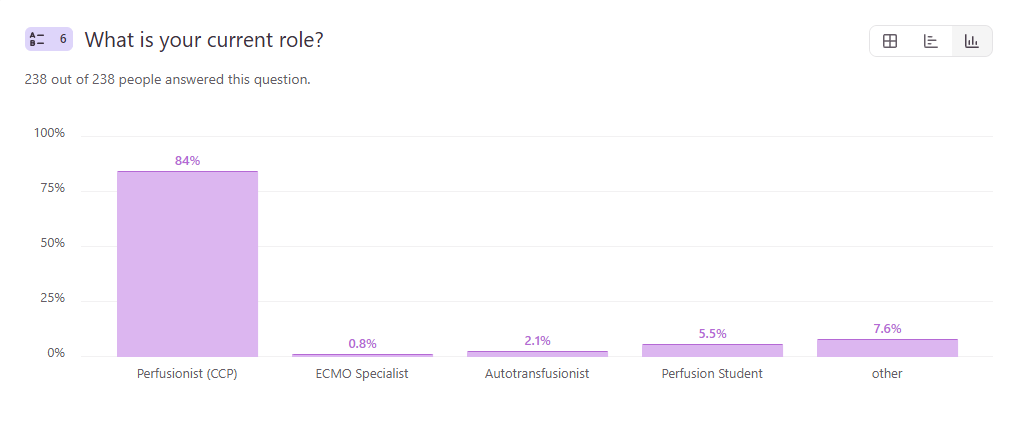
Responses by Age Group
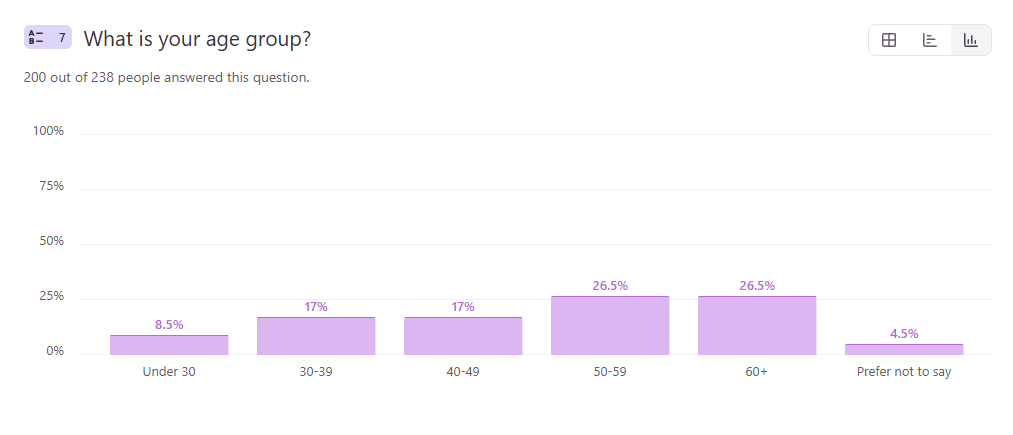
Question 1: Replacing Animal Models
At first glance, the results suggest a clear shift toward simulation, with 47.7% of respondents supporting the replacement of animal testing. However, the remaining responses tell a more nuanced story. Nearly as many respondents selected either “yes, in certain cases” or “it depends,” indicating that while simulation is gaining traction, full replacement is far from universally accepted.
This divide reflects a broader tension between ethical progress and clinical confidence. Many respondents appear to support reducing or eliminating animal use in principle, but hesitate when it comes to specific applications where realism, unpredictability, or high-risk learning is involved. In practice, this suggests that simulation is viewed as a strong complement, but not yet a universal substitute, particularly in complex or exploratory scenarios.
Question 2: Confidence in Simulation Technology
Confidence in simulation technology lands firmly in the middle. While 43.2% of respondents report being somewhat confident, only 20.5% describe themselves as very confident. At the same time, over a third of respondents fall into neutral or low-confidence categories, signaling that trust in simulation is still developing.
This distribution suggests that simulation has reached a level of acceptance, but not complete credibility. For many, it is reliable enough for training and reinforcement, but not yet robust enough to fully replace higher-stakes or less predictable learning environments. The gap between “somewhat” and “very” confident is especially telling, pointing to a need for continued improvements in realism, consistency, and clinical applicability before broader trust can be achieved.
Question 3: Experience with Animal Models
With 63.8% of respondents reporting direct experience with animal models, it is clear that this method remains deeply embedded in perfusion training and research. This exposure likely plays a significant role in shaping how simulation is evaluated.
For those who have worked in animal labs, the comparison is not theoretical. It is grounded in a firsthand understanding of physiological response, procedural complexity, and the weight of real-world consequences. This may help explain why many respondents are cautious about full replacement, as their benchmark for realism is based on lived experience rather than simulation alone.
Question 4: What Matters Most
When asked what should carry the most weight in this decision, respondents were nearly split between ethical considerations (39.7%) and translational accuracy and patient safety (36.8%). This close margin highlights the core challenge at the center of the debate.
On one hand, there is a clear desire to move toward more ethical, non-animal-based approaches. On the other hand, there is an equally strong emphasis on ensuring that training methods translate effectively to patient care. Educational effectiveness, while still important, ranks behind these two priorities, suggesting that outcomes and ethics take precedence over methodology alone. Together, these results reinforce that decisions around simulation and animal models are not driven by a single factor, but by the need to balance values with real-world impact.
Question 5: What Needs to Improve in Simulation Before It Could Fully Replace Animal Models?
Responses to this question reveal a clear theme: simulation must better replicate the complexity, variability, and consequences of real-life clinical scenarios before it can fully replace animal models.
Many respondents pointed to the need for greater physiological realism and responsiveness. As one noted, “A mimic of physiologic response that could respond to complex molecular signaling,” while another emphasized improving technical performance: “Realism. Smooth out glitches.” These comments reflect a desire for simulation to more closely mirror how the body reacts under dynamic and unpredictable conditions.
Others highlighted the importance of capturing the stakes of real-world decision-making. One respondent shared, “When you have an accident in an animal lab, you see the real-life consequences. That can’t be duplicated in a sim lab where you can just start over.” Similarly, another noted, “There’s no way to simulate a true life and death situation… It’s something that weighs in the back of your mind when you know a life is on the line.” These perspectives suggest that, beyond technical improvements, simulation must also address the psychological and experiential aspects of clinical training.
Accessibility and practicality also surfaced as key considerations. Respondents pointed out that cost and availability can limit adoption, with one noting that simulation is sometimes “too expensive” for widespread use. Others emphasized the need for broader access across training programs to ensure consistency in education.
At the same time, several respondents questioned whether simulation could ever fully replace animal models. Comments such as “You can’t replicate life” and “In certain type[s] of studies, simulation models cannot replace animal models” reflect a belief that there are inherent limitations to simulation, particularly when exploring unknown or complex physiological responses.
Taken together, these responses highlight both optimism and skepticism. While many see simulation as the future, there is a clear expectation that it must continue to evolve significantly before it can fully match the depth and realism of live models.
Reflections on Simulation in Perfusion
This month’s poll highlights a profession navigating the intersection of innovation and experience. While simulation is widely supported and continues to improve, many perfusionists remain cautious about fully replacing animal models, particularly in high-stakes or exploratory settings. The conversation is not simply about choosing one over the other, but about understanding where each approach adds value.
As technology advances, expectations will continue to rise. For now, the responses suggest that simulation is an essential and growing part of perfusion training, but not yet a complete replacement. The future will likely depend on how well it can bridge the gap between technical capability and clinical reality.
Stay tuned for the next Pulse on Perfusion as the series continues to share insights from across the community.
Appendix of Additional Insights
- Younger respondents show the strongest support for replacing animal testing, with over half of those under 40 selecting “no” to animal use (Under 30: 52.94%; 30–39: 54.55%). Older groups remain more mixed, particularly among those 60+, where “it depends” responses increase (31.37%).
- Confidence in simulation aligns with attitudes toward replacement. Among those who support replacing animal models, a higher percentage report being very confident (32.74%), while those who support continued use tend to fall into neutral or lower confidence categories.
- Direct experience with animal models influences perspective. Among respondents who support continued use in certain cases, 78.13% have participated in animal-based training, suggesting firsthand experience reinforces perceived value.
- “It depends” respondents reflect a more flexible, context-driven mindset, with moderate confidence levels and mixed experience, indicating a tendency to weigh multiple factors rather than take a definitive stance.
